To diagnosis BA, many tests must be done before a conclusive diagnosis can be made. These tests may include blood and liver tests, an ultrasound examination, X-rays, and a liver biopsy. During a liver biopsy, small amount of liver tissue is removed with a needle for examination of biliary ducts. Typically, a "normal" piece of liver would show very small amounts of biliary ducts along with arteries and veins. A suspected BA liver sample would show a greater number of biliary ducts. This is the body's way of compensating for the blockage in the biliary duct system/ tree.
Finally, a cholangiogram will be performed to provide a definitive diagnosis. The procedure is done by injecting dye into the bile ducts under continuous imaging. Any blockage will prevent the dye from advancing further along the biliary tree and lead to the diagnosis of BA.
Finally, a cholangiogram will be performed to provide a definitive diagnosis. The procedure is done by injecting dye into the bile ducts under continuous imaging. Any blockage will prevent the dye from advancing further along the biliary tree and lead to the diagnosis of BA.
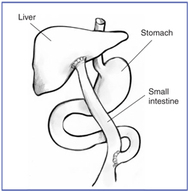
Sadly, there is no cure for biliary atresia. The only treatment is a surgical procedure called the Kasai. This procedure removes the blocked bile ducts outside the liver and replaces them with a portion of the baby’s own intestine, which acts as a new duct. The goal or outcome of the Kasai procedure is to allow drainage of bile from the liver into the intestine through the new "two way" duct.
The operation is completely or partially successful about 80 percent of the time if performed early (before 3 months of age). In babies who respond well, jaundice and other symptoms usually disappear after several weeks.
In cases where the Kasai procedure does not work, the problem often lies in the blocked bile ducts that are inside the liver. Only a liver transplant can help solve this problem. A suitable donor organ must be found quickly, before damage to the liver from the backed-up bile becomes deadly.
In the cases where the Kasai procedure is successful, the child may recover and live a normal life. However, in most cases, even when surgery is successful, there are still a number of ways in which the liver can suffer damage. One way may happen due to the "two way" duct. Unlike the native biliary duct system, the newly attach intestine does not prevent all "back flow" into the liver, which causes scarring and damage of the liver. Damage can also occur due to a gradual inflammation of the bile ducts present inside the liver. This will cause a build up of bile within the liver over time.
All BA fighters will need monthly/ weekly specialized medical care, frequent testing of blood and examinations, daily medications and infection prevention.
http://www.liverfoundation.org/abouttheliver/info/biliaryatresia/#Q6
The operation is completely or partially successful about 80 percent of the time if performed early (before 3 months of age). In babies who respond well, jaundice and other symptoms usually disappear after several weeks.
In cases where the Kasai procedure does not work, the problem often lies in the blocked bile ducts that are inside the liver. Only a liver transplant can help solve this problem. A suitable donor organ must be found quickly, before damage to the liver from the backed-up bile becomes deadly.
In the cases where the Kasai procedure is successful, the child may recover and live a normal life. However, in most cases, even when surgery is successful, there are still a number of ways in which the liver can suffer damage. One way may happen due to the "two way" duct. Unlike the native biliary duct system, the newly attach intestine does not prevent all "back flow" into the liver, which causes scarring and damage of the liver. Damage can also occur due to a gradual inflammation of the bile ducts present inside the liver. This will cause a build up of bile within the liver over time.
All BA fighters will need monthly/ weekly specialized medical care, frequent testing of blood and examinations, daily medications and infection prevention.
http://www.liverfoundation.org/abouttheliver/info/biliaryatresia/#Q6